
Humber and North Yorkshire Cancer Alliance has funded a new short film which highlights the experiences of people with a cancer diagnosis.
KPOW! (Know the Power of Words) shines a light on the importance of language used by clinicians during diagnosis and treatment.
The film, which the Cancer Alliance co-funded with Macmillan Cancer Support, received its premiere at Hull Truck Theatre on Monday 8th July. After the showing, members of the cast and crew took part in a Q & A session with the attendees.

You can now view KPOW! on the Cancer Alliance’s YouTube channel, here.
KPOW! co-stars and was written by North Yorkshire playwright Libby Pearson. In the film, Libby is one of four friends openly discussing experiences of cancer, and how the way medical and nursing staff spoke and acted towards them during their treatment and care had consequences on their emotions.
The film also stars Allyson Kent, a former NHS worker, who lives in the East Riding of Yorkshire. Allyson was diagnosed with breast cancer in 2019 and ovarian cancer in 2020 and is now a Cancer Alliance patient representative.
In KPOW!, Libby, Allyson, Hannah Coysh and Rosie Hamblyn talk about their hope that negative statements can be reconsidered and reframed to be more sensitive and positive.
Even common words such as “but”, “however”, “until” and “yet” can affect patients living with cancer. Libby, InkBlot Films and the cast hope that their film can inspire clinicians to take the time to consider how their words and actions can leave a lasting, negative impression on their patients.
The four friends in KPOW! have all been affected by cancer in different ways. Libby lost her father to cancer, Allyson is living with cancer and is a patient representative for the Cancer Alliance, Hannah is a Macmillan doctor, and Rosie is a cancer survivor.

As they chat about their feelings, they all reveal a shared desire for words to be delivered with kindness and compassion, using clear explanations and active language, with eye contact.
KPOW! combines humour and poignancy to deliver a very potent message of the need for understanding and respect when living with cancer.
The film was originally conceived and commissioned as a play by Libby, specially written for a Living with and Beyond Cancer conference organised and facilitated by Macmillan GPs Dr Hannah Coysh and Dr Kate Thomas in June 2023. Although visually different, the concept of the film, directed by Jay Sillence of InkBlot FIlms, remains the same.
Libby said: “As a theatre-maker specialising in issue-based work – particularly around health and equality – I believe theatre and film are such strong tools in helping people reflect on their own beliefs and behaviour. They can make a huge impact and effect positive change.
“Making a film was new to almost everyone in the room and the nerves were palpable, but Jay and his team helped transform those nerves into a positive energy that really comes through in the film. Even though the day was long and very tiring, we’d have done it all again the next day.
“The scenes with Allyson running were fabulous. I scouted the locations and everywhere I turned was a flooded road or a boggy field. Ally and Jay had to negotiate sheep, bogs and tooting cars, but the results are great. Jay, like Ginger Rogers, had to do everything Ally did, but backwards, without the heels!
“I am hoping that anyone who sees the film, be they health professionals in any role, or those supporting people living with cancer, will consider what they say and how they say it. Think about the impact of words, and truly put the patient at the centre of the conversation.”
Allyson added: “I worked in the NHS for the whole of my career and am now experiencing life as a patient. Having a cancer diagnosis is life-changing at every level, and words matter. They can give hope or cause real harm. I will never forget those words used that day, and how they made me feel. I am much more sensitive to the words people use now.
“Normally I’m a very private person, but I want to share my story to make people think about the language they use or how a lack of words impact on patients.”
On the making of the film, Allyson said: “What an experience! So much behind the scenes work… lighting… fluffing words! The fun of creating something together was an amazing experience and we laughed so much, even though it was a long, long day and we were tired, but we didn’t stop, we didn’t give in.
“It was an emotional day for me as this is real, this was my story, but I am so proud of what we have achieved.”
Lucy Turner, Managing Director of Humber and North Yorkshire Cancer Alliance, said: “We are so proud of Libby’s film, the cast’s performances and Jay’s hard work in making KPOW! The subject matter is very close to our hearts, and we are thrilled that we’ve played a part in the process of highlighting this important issue.
We hope medical and nursing staff will take on board the words used by Libby, Allyson, Hannah and Rosie, and consider how important the language and actions they use with cancer patients are. They can stay with a patient forever.”
KPOW! (Know the Power of Words) is now available on the Cancer Alliance YouTube channel, here. Please share across your network, particularly with frontline staff who have clinical and non-clinical contact with patients, including:
- doctors
- nurses
- paramedics
- social workers
- care workers









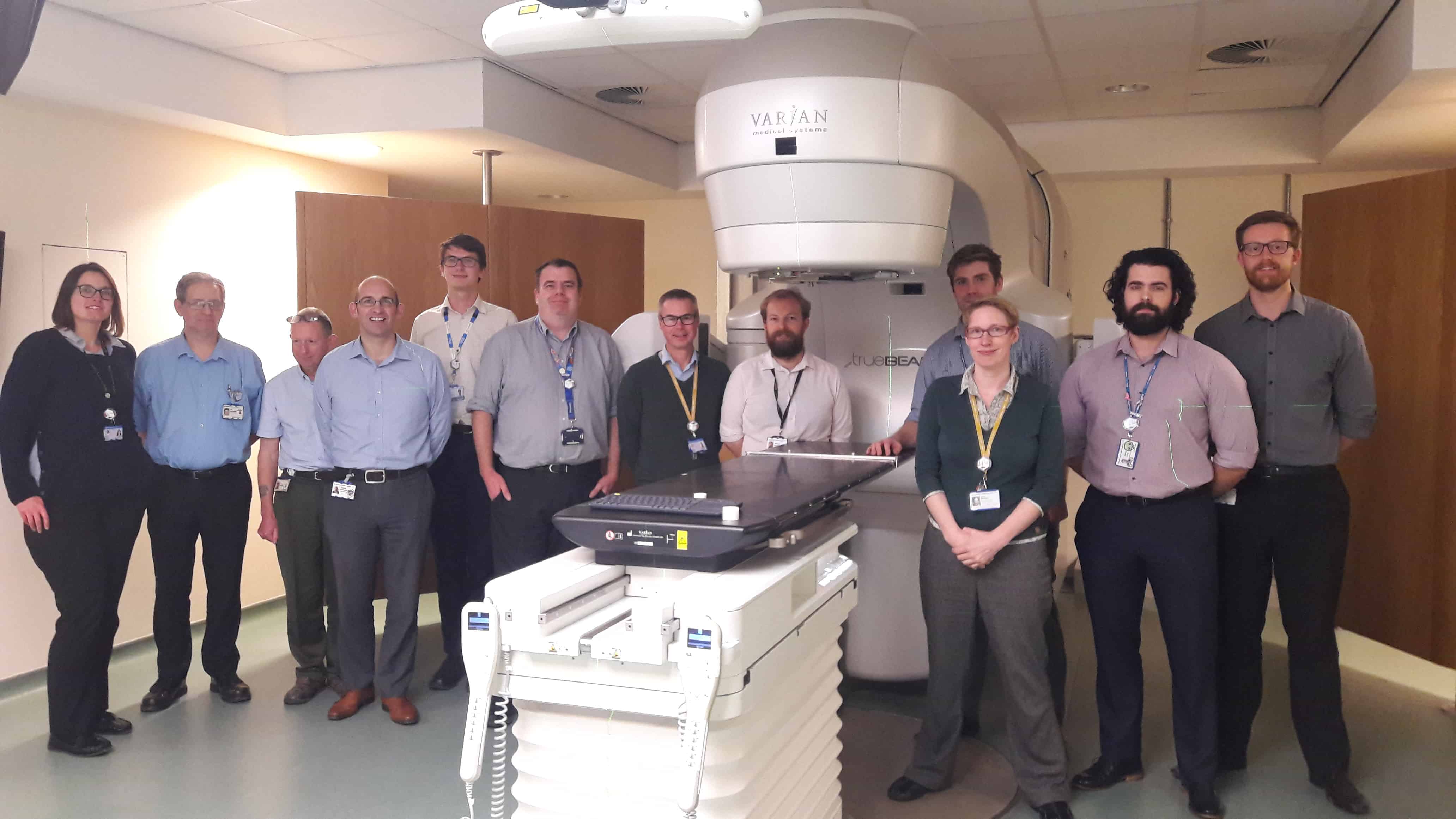
 Now the 36-strong team are the first radiotherapy physics team in the country to achieve service standard BS 70000:2017, assuring patients around the quality and safety of the service they’re receiving and the competence of staff delivering treatment.
Now the 36-strong team are the first radiotherapy physics team in the country to achieve service standard BS 70000:2017, assuring patients around the quality and safety of the service they’re receiving and the competence of staff delivering treatment.